The following are some terms and acronyms commonly used by AIDS service providers, advocates, domestic violence service providers, policymakers, researchers, and academics. It is helpful to develop familiarity with these terms when helping survivors discuss options, negotiate medical regimes, talk to other service providers, or engage in advocacy. The "jump to" box below will take you to full definitions that are listed at the end of this collection.
- AIDS
A disease of the immune system due to infection with HIV. HIV destroys the CD4 cells of the immune system, leaving the body vulnerable to life-threatening infections and cancers. Acquired immunodeficiency syndrome (AIDS) is the most advanced stage of HIV infection. AIDS is the stage in HIV infection, when the immune system is most compromised and damaged, leaving it unable to fight off infection. The infections are referred to as opportunistic infections. AIDS is defined as 1. Having a CD4 count below 200 cells per cubic millimeter of blood (200 cells/mm3), or 2. Developing an opportunistic infection regardless of CD 4 count. (See also CD4, HIV, Opportunistic Infections) (AIDSinfo, U.S. Department of Health and Human Services) - AIDS Drugs Assistance Program (ADAP)
ADAP provides medications for the treatment of HIV disease. Program funds may also be used to purchase health insurance for eligible clients and for services that enhance access to, adherence to, and monitoring of drug treatments (Health Resources and Services Administration). - Adherence (Medical Adherence/Treatment Adherence)
Treatment adherence, sometimes called medical adherence, is a commonly used term meaning, “to take medication as directed”, when and how it is instructed. Treatment adherence is important because it can decrease viral load, and prevent drug resistance. (See also: Viral Load, Drug Resistance) - AIDS Service Organization (ASO)
ASOs are community support agencies providing emotional support, resources, case management, and medical services for people living with HIV/AIDS and often the family members and partners of people living with HIV/AIDS. They may provide a wide variety of services, including helping clients apply for ADAP (See also ADAP) or other social benefits, group therapy, connecting clients to mental health networks, or even storing medication. - Antiretroviral Therapy (ART)
ART is the treatment regimen, or the recommended treatment for HIV infection. Antiretroviral therapy (ART) involves using a combination of three or more antiretroviral (ARV) drugs from at least two different HIV drug classes to prevent HIV from replicating (AIDSinfo, U.S. Department of Health and Human Services). (See also: Drug Class) - Medical Case Management
Medical case management is a support service often provided at AIDS Service Organizations. It includes a diverse array of services designed to minimize barriers to adhering to medical treatment for people living with HIV/AIDS. This may include linking clients with health care, following up on appointments and helping clients track and monitor outcomes of medical treatment (through tracking viral load, and CD4 count). Medical case management also includes supporting clients in getting other types of needs met through personal support systems, public benefits, insurance, and psychosocial support in order to facilitate the highest possibility of treatment adherence. - CD-4 Count (T-cell count)
A laboratory test that measures the number of CD4 T lymphocytes (CD4 cells) in a sample of blood. In people with HIV, the CD4 count is the most important laboratory indicator of immune function and the strongest predictor of HIV progression. The CD4 count is one of the factors used to determine when to start antiretroviral therapy (ART). The CD4 count is also used to monitor response to ART (AIDSinfo, U.S. Department of Health and Human Services). (See also T-cell) - Continuum of Care
The HIV care continuum—sometimes also referred to as the HIV treatment cascade—is a model that outlines the sequential steps or stages of HIV medical care that people living with HIV go through from initial diagnosis to achieving the goal of viral suppression (a very low level of HIV in the body), and shows the proportion of individuals living with HIV who are engaged at each stage (https://www.aids.gov/federal-resources/policies/care-continuum/) - Drug Class
A group of drugs that share common properties, which may include a similar mechanism of action, chemical structure, or approved use. Antiretroviral (ARV) HIV drugs are classified into six drug classes on the basis of how each drug interferes with the HIV life cycle. These six classes include the nucleoside reverse transcriptase inhibitors (NRTIs), non-nucleoside reverse transcriptase inhibitors (NNRTIs), protease inhibitors (PIs), fusion inhibitors, CCR5 antagonists, and integrase strand transfer inhibitors (INSTIs) (AIDSinfo, U.S. Department of Health and Human Services). - (Drug) Resistance
The HIV virus makes millions of copies of itself once it enters the human body. Sometimes, the virus mutates (changes form) and makes varying copies of itself. If a person living with HIV is on antiretroviral therapy (ART), and the HIV virus mutates, the HIV medications may no longer work to fight these mutated cells. This may cause HIV treatment to fail. Treatment adherence is very important to HIV control. It is important that medications are taken exactly as prescribed. The higher the number of HIV cells that replicate in the body, the more likelihood of cells mutating and becoming resistant to treatment. (See also ART, Medical Adherence) - Female Condom
The female condom, sometimes marketed as the FC2, is a woman-controlled (and in the case of anal sex, receptive partner-controlled) barrier method for preventing pregnancies and STIs. It is made of nitrile, and can be inserted into the vagina up to 8 hours before sex. It is the only receptive partner-controlled barrier method that may prevent both STIs and pregnancy. It is often thought of as an alternative, or additional tool for women whose male partners are reluctant to utilize male condoms. (Planned Parenthood) - HIV
HIV is the human immunodeficiency virus. It is the virus that can lead to acquired immunodeficiency syndrome, or AIDS. HIV attacks the immune system protecting white blood cells in the human body and destroys them so they can no longer effectively fight off diseases and infections. Without proper treatment, HIV may lead to AIDS (AVERT). (See also AIDS) - Health Resources and Services Administration (HRSA)
HRSA is the primary Federal agency for improving access to health care services for people who are uninsured, isolated, or medically vulnerable. HRSA funds the Ryan White Program, which provides a majority of funding for ASOs, and community medical clinics providing services to people living with AIDS. (See also Ryan White HIV/AIDS Program) - HIV Life (replication) Cycle
The HIV life cycle is the 7-step process HIV uses to replicate itself in the body. First, it attaches itself to the surface of the white blood cells through a process called binding, then it fuses with the cell allowing it to sneakily enter the white blood cell in a process called fusion. Throughout the 7 steps of the life-cycle, HIV’s goal is to make more and more copies of itself. Antiretroviral treatment is a combination of medications in different drug classes which fight HIV during different parts of the life cycle. (See also ART, Drug Classes)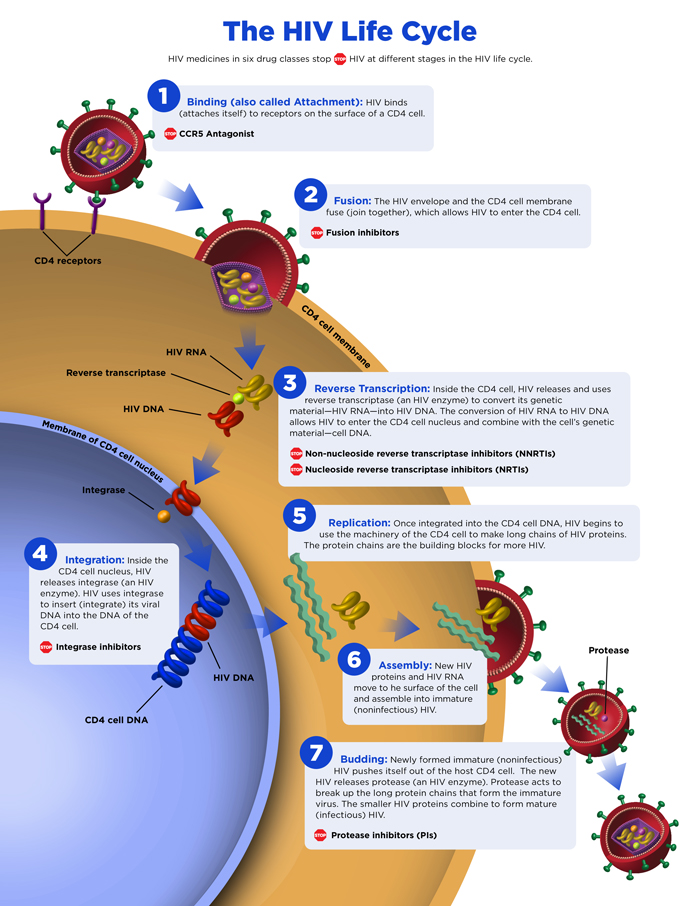
- Mother to Child (Perinatal) Transmission
Mother to child transmission of HIV describes the process of HIV positive mothers passing HIV on to their children through pregnancy, labor/childbirth, or through breastfeeding. Women with HIV who take antiretroviral medication during pregnancy as recommended can reduce the risk of transmitting HIV to their babies to less than 1%. Since the mid-1990s, HIV testing and preventive interventions have resulted in more than a 90% decline in the number of children perinatally infected with HIV in the United States. (Centers for Disease Control and Prevention) - Non-Occupational Post-Exposure Prophylaxis (nPEP)
Short-term treatment started as soon as possible after high-risk non- occupational exposure to an infectious agent, such as HIV, hepatitis B virus (HBV), or hepatitis C virus (HCV). Non-occupational exposure refers to exposure to an infectious agent that occurs outside of one’s work. The purpose of non-occupational post-exposure prophylaxis (nPEP) is to reduce the risk of infection. (AIDSinfo, U.S. Department of Health and Human Services) - Opportunistic Infection
People with healthy immune systems can be exposed to certain viruses, bacteria, or parasites and have no reaction to them—but people living with HIV/AIDS can face serious health threats from what are known as “opportunistic” infections (OIs). These infections are called “opportunistic” because they take advantage of weakened immune systems, and they can cause devastating illnesses. OIs are signs of a declining immune system. Most life-threatening OIs occur when the CD4 count is below 200 cells/mm3. OIs are the most common cause of death for people with HIV/AIDS. The CDC has developed a list of more than 20 OIs that are considered AIDS-defining conditions—if a person is living with HIV and has one or more OI, they will be diagnosed with AIDS, no matter what the CD4 count happens to be (AIDS.gov). (See also, AIDS, CD4 Count) - People Living with HIV/AIDS PLWA (PLWHA)
People across the span of gender, race, ability, sexuality and age from infancy to adulthood who are infected with HIV/AIDS. - Post-Exposure Prophylaxis (PEP)
Short-term treatment started as soon as possible after high-risk exposure to an infectious agent, such as HIV, hepatitis B virus (HBV), or hepatitis C virus (HCV). The purpose of post-exposure prophylaxis (PEP) is to reduce the risk of infection. An example of a high-risk exposure is exposure to an infectious agent as the result of unprotected sex. (AIDSinfo, U.S. Department of Health and Human Services) - Pre-Exposure Prophylaxis (PrEP)
PrEP is an HIV risk reduction tool for HIV negative people at who are at high risk of contracting HIV. The medication used is called Truvada, and it can drastically reduce (up to 92%) the transmission of HIV when used with other safer sex practices like condoms, or with clean needles in the case of people who inject drugs. PrEP is very effective when taken consistently, and is typically prescribed to people who inject drugs, men who sleep with men (MSM), and women who are HIV negative but have HIV positive male partners. People who use PrEP must commit to frequent medical check-ups as often as every three months, and must take medicine exactly as prescribed. - Rapid Test
A type of HIV antibody test used to screen for HIV infection. A rapid HIV antibody test can detect HIV in blood or oral fluid in less than 30 minutes. A positive rapid HIV antibody test must be confirmed by a second test for a person to be definitively diagnosed with HIV infection. (AIDSinfo, U.S. Department of Health and Human Services) - Ryan White HIV/AIDS Program
The Ryan White HIV/AIDS Program works with cities, states, and local community-based organizations to provide services to an estimated 536,000 people each year who do not have sufficient health care coverage or financial resources to cope with HIV disease. The majority of Ryan White HIV/AIDS Program funds support primary medical care and essential support services. A smaller but equally critical portion is used to fund technical assistance, clinical training, and the development of innovative models of care. The Ryan White HIV/AIDS Program, first authorized in 1990, is administered by the U.S. Department of Health and Human Services (HHS), Health Resources and Services Administration (HRSA), HIV/AIDS Bureau (HAB) (Health Resources and Services Administration). (See also HRSA) - Sexually Transmitted Disease/Infection
Sexually transmitted diseases (STDs) are caused by infections that are passed from one person to another during sexual contact. This is why the term STD and STI are often used interchangeably. It is important to note that having an STD increases risk for contracting HIV. This is because the same behaviors and circumstances that may put a person at risk for getting an STD can also put them at greater risk for getting HIV. Additionally, open wounds or sores as a result of an STD increase the likelihood of contracting of HIV. Finally, if a partner has HIV and an STD, there are likely more HIV cells in their blood (they have a high viral load), making their ability to transmit the disease to an HIV-negative partner much higher. (Centers for Disease Control and Prevention) (See also Viral Load) - T-cells (White Blood Cells)
The terms “CD4 cell” and “T-cell” both refer to the same type of cell—a CD4 T lymphocyte—and are often used interchangeably. CD4 cells or T-cells are a type of white blood cells that play a major role in protecting your body from infection. They send signals to activate your body’s immune response when they detect “intruders,” like viruses or bacteria. Once a person is infected with HIV, the virus begins to attack and destroy the CD4 cells of the person’s immune system. HIV uses the machinery of the CD4 cells to multiply (make copies of itself) and spread throughout the body. (AIDS.gov) (See also HIV Life Cycle, CD4 count) - Transgender
Transgender is a term used to describe people whose gender identity differs from the sex the doctor marked on their birth certificate. Gender identity is a person's internal, personal sense of being a man or a woman (or someone outside of that gender binary). For transgender people, the sex they were assigned at birth and their own internal gender identity do not match. People in the transgender community may describe themselves using one (or more) of a wide variety of terms, including (but not limited to) transgender, transsexual, and genderqueer. Always use the term preferred by the individual. (GLAAD) - Treatment Regime
A structured treatment plan designed to improve and maintain health. Recommended HIV treatment regimens include a combination of three or more antiretroviral drugs from at least two different drug classes. (AIDSinfo, U.S. Department of Health and Human Services) (See also ART, Drug Classes, HIV Life cycle) - Viral Load (Undetectable Viral Load)
The viral load is a term used to describe the amount of virus in the blood of a person with HIV. A higher viral load means there is more HIV in the body and fewer white blood CD-4 cells to fight infection. A low viral load can get to levels called “undetectable.” An undetectable viral load does not mean the HIV is cured, or that there is no HIV in the body. It means that the amount is so low, that it cannot be measured with standard lab test. Having an undetectable viral load greatly lowers the risk of transmission, and greatly improves the health of the person living with HIV.









